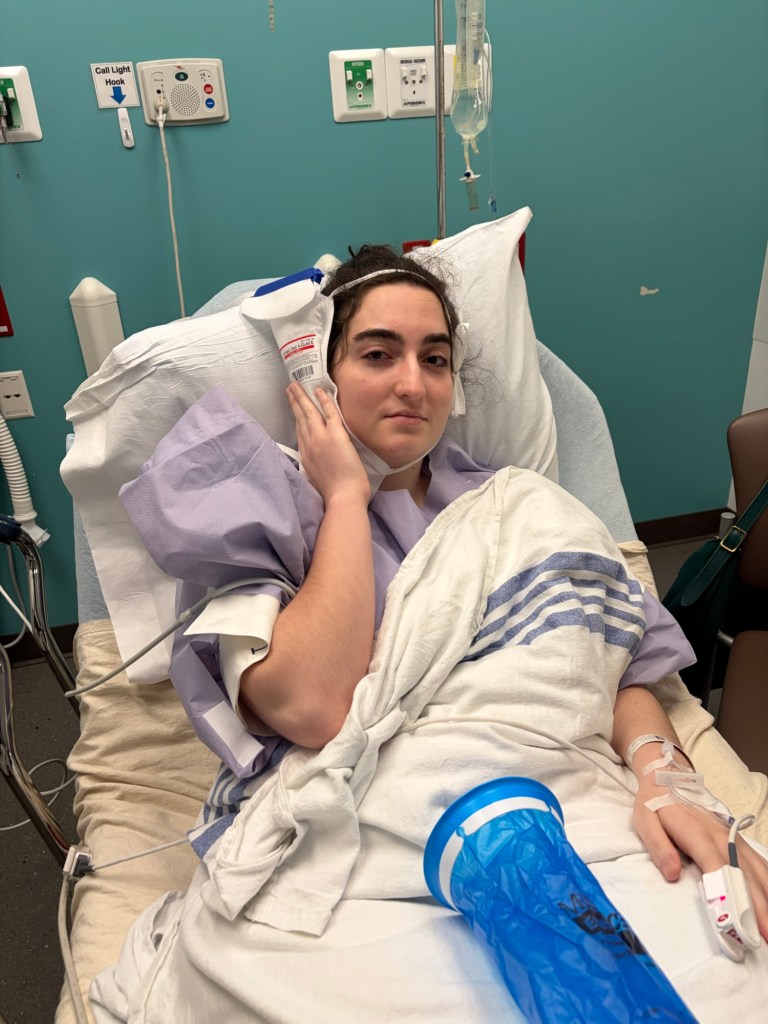
Thank you for praying for me. The jaw surgery went very well with no complications, and I was able to go home the same day. About 5½ months ago, I yawned and my jaw popped and became stuck open. I was able to force my mouth closed (I know now not to do that in the future 😅). I went to the dentist, my doctor, and an ENT, but they all told me it was outside their specialties. I’ve only been able to open my mouth about one and a half fingers wide. It’s a type of locked jaw.
It wasn’t as bad, but a few years ago I had something similar happen to my jaw (also from a yawn) and was sent to an oral surgeon at OHSU. Since it was still within the timeframe, I was able to see the same oral surgeon as before. He measured my jaw opening, which was much more restricted this time. He knew exactly what the problem was and how to fix it with a relatively small procedure. I told him I was so happy he had a plan because I wasn’t sure who I would go to next. He smiled and replied that he was it.
The surgery has an over 80% success rate, but it really needs to be done within six months to work best. Insurance wasn’t helpful, so I pushed to get in about three months into this and had the surgery at 5½ months. It was close, but getting in felt like an answered prayer. I’m very hopeful it will work. The surgeon told me he has never had to repeat one of these procedures.
Here’s what they did: I was placed under sedation rather than general anesthesia because the surgery was only about 30 minutes. Anesthesia didn’t want to risk the complications of putting me fully under, especially since I would have needed intubation and my mouth wasn’t opening all the way. There was a lot of logistics involved because of my medical history—I’m allergic to some medications they use with anesthesia, and the fusion in my neck (plus the hardware) made them extra cautious. If there had been an emergency need to intubate, they had a special “blade” type tool ready. I didn’t ask for more details on that one.
The plan was to start with sedation. The surgeon told me I would be asleep and wouldn’t remember anything. But when his team came in, they said I would be awake enough to be aware, talk with them, and respond. I really didn’t want to be awake, remember anything, or feel any pain. They promised they would watch my body for signs of distress and adjust the medications as needed.
It was a minor surgery, so it was just my mom and me at the hospital. We prayed together before leaving the house. I had no idea what to expect because I’m used to much higher-stress, more complicated surgeries. We thought it would be easier with fewer people there so it wouldn’t be as triggering for me. I wasn’t prepared for the whole team coming into my room at different times for introductions. It makes sense that it’s standard procedure, but it brought up a lot of emotions and made the two hour wait in the prep area feel agonizing.
When I was finally taken back to the surgical room, I was more than ready. They tucked me in with warm blankets and gave me the anesthesia. The surgeon explained that they were going to take really good care of me. He said it was a simple procedure compared to the surgeries he usually does and that my jaw would have relief soon.
They inserted two needles into my jaw joint, drained the inflammatory fluid, and irrigated it to cleanse the joint. Then he dislocated my jaw and repositioned it correctly. The joint was filled with saline to keep it in place because it was misshapen. The surgeon told me to think of it like a balloon that needed to be refilled. Finally, he injected a steroid into the joint to help with swelling. So in the end, I just have two small needle marks by my ear and a very tender mouth from all the stretching and repositioning.
A few weeks before surgery, the surgeon squeezed me into his schedule and gave me a steroid injection in the joint to help with the pain while waiting. It took the edge off, but I still couldn’t open my mouth much. A week before surgery, I could feel it starting to wear off.
I remember waking up in a room with a box of tissues in my lap, weeping. I’ve never come out of anesthesia without turning into an emotional wreck. I get super gushy and love everyone. Once I became aware of what I was saying, I was crying to my mom about how nice everyone had been. When I got my bearings, she took the tissue box away and we laughed. We’ve been through this six times now—wisdom teeth, tonsil removal, and brain surgeries.
I had to stay in the hospital a few extra hours to get my pain under control. When I came home, a dear family friend had a homemade dinner waiting. I ate some cake, fell asleep on the couch, then woke up later and had some pasta. I’m on a very soft food diet for the next two weeks and doing a ton of icing on my jaw. The doctor said ice will bring the most relief.
The theory is that having C1 removed and not fused, with undiagnosed hEDS led to instability in my neck. Then four months in the the full cervical collar neck brace caused my neck muscles to weaken, which threw my jaw out of place. The oral surgeon told me this is a common issue for young women with hEDS.
I’ve also been having horrible vertigo—worse than I’ve ever experienced. I went to the ER a couple of weeks ago, where they did scans and gave me some meds. I’ve had the Epley Maneuver (or as they call it, the “Barbecue Maneuver”) done three times now, and it has helped significantly. It’s hard to know whether the vertigo is coming from my jaw, my neck, migraines, the loose crystals in my ears, or all of the above—it’s all tangled together.
Hopefully my body starts to calm down and the symptoms ease up. I’ve also had very blurry vision and double vision, so I’m in the process of getting a referral to the Casey Eye Institute for a neuro-ophthalmology evaluation.
It’s been a rough few months with a lot of pain and having to adapt to life with very limited jaw movement. But as soon as I woke up from surgery, I could open my mouth almost normally again. It’s still swollen and aggravated (there may be some saline still trapped from the flushing), but as it heals I should get even more movement. I was expecting a lot of bruising and maybe scabs, but you can’t even see anything. I just have a small Band-Aid. It feels like a tender mosquito bite. I threw up last night from pain, but sleeping with an ice pack is making it manageable.
There are so many things to be thankful for these last few months: being able to call my Uncle Frank (a retired dentist), who helped us make a plan and get on the right path; so many church family and friends praying; and a home-cooked meal waiting when we got home. 💗
It’s been a hard-won lesson, but there’s always joy and peace to be found in the waiting—whether you’re waiting for healing, surgery, or something else that causes that deep longing in your heart. God is always there. I’ve said so many prayers that felt like echoes of previous ones, like I was knocking on a worn-out door in Heaven. But even when the wait is long or the answer doesn’t come right away or in the way we expect, God is walking with us through this complicated journey we call life. Lately, the story of the Shepherd and the 99 has been rattling around in my mind—maybe because I’ve felt like that one lost sheep. Not by choice, but because of circumstances.
Chronic Illness can cut you off from what you know. It robs you of your strength and makes the simplest things, like getting ready to leave the house, feel like mountains. It’s isolating. It’s giving me time to know my Shepherd. For when I walk through the Valley of the Shadow He is still with me.
Blessings,
Shae
Psalm 23










